
Digestive Disorders: Modern Challenges and EmergingPerspectives
Most of us go about our days without giving a second thought todigestion—until something goes wrong. Yet for millions ofAmericans, digestive disorders are a persistent, sometimesinvisible burden that can disrupt work, sleep, social life, andoverall wellbeing.
The spectrum of digestive disorders is broad, running from therelatively common (acid reflux, constipation, irritable bowelsyndrome) to more complex and chronic conditions like Crohn’sdisease. Even something as seemingly benign as heartburn can, iffrequent, wear down quality of life. Meanwhile, symptoms likecramping, bloating, diarrhea, or gastrointestinal bleeding cansignal more serious concerns. Left unaddressed, persistentdigestive dysfunction may chip away at general health, and in rarecases, become life-threatening.
By downloading the Digital Patient Chart mobile app you can better control your patient portal.
Why Digestive Disorders Happen
The digestive tract is a marvel of biology, but it’s alsosurprisingly sensitive. Stress, diet, infections, genetics, immunedysfunction, and disruptions in the gut-brain axis can all play arole. Increasingly, research points to the nervoussystem—especially the communication superhighway between the brain,brain stem, and gut—as a key player in both the development andpersistence of digestive symptoms.
The vagus nerve, for example, acts as a critical relay betweenthe brain stem and the gastrointestinal (GI) tract, regulatingeverything from stomach acid production to intestinal motility. Ifthis neural circuitry falls out of sync—due to injury, chronicstress, or even subtle spinal misalignments—some patients mayexperience a cascade of digestive issues. These connections are thefocus of growing scientific attention, with the so-called"gut-brain axis" now a buzzword in both research and clinicalcircles.
Current Approaches to Treatment
For many, the first response to digestive discomfort is a tripto the pharmacy—antacids, laxatives, or anti-diarrheals are commonover-the-counter fixes. If symptoms persist, physicians mayprescribe medications ranging from proton pump inhibitors tobiologics or steroids, depending on the diagnosis. In severe orrefractory cases, surgery may be considered.
Yet, these interventions are not without risk. Side effects caninclude further digestive upset, immune suppression, or, in thecase of surgery, significant recovery time and lifestyle changes.It’s no surprise that many patients seek complementary orintegrative approaches to manage their symptoms and support theiroverall health.
The Nervous System–Digestive System Connection
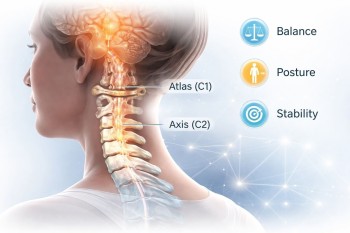
A fascinating area of ongoing research explores how spinalalignment, particularly in the upper cervical region (the top ofthe neck), might influence digestive health. The theory goes likethis: misalignments in the upper cervical spine can impact brainstem function, which in turn may disrupt the signals sent via thevagus nerve to the gut. While this idea is still underinvestigation, some patients and clinicians report meaningfulimprovements in digestive symptoms following gentle, targetedchiropractic adjustments.
It's important to note that chiropractic care, including uppercervical techniques, is not a cure-all. Scientific evidence isstill evolving, and results can vary. That said, for individualswho haven’t found relief through conventional means, exploring thenervous system’s role in gut health is increasingly recognized as areasonable adjunct—not a replacement—for medical management.
A Patient-Centered Perspective
Dr. Jerome Ri, DC, of Upper Cervical Health Care of OrangeCounty, is one practitioner who specializes in this integrativeapproach. Drawing on years of focused training in the brain stemand upper cervical spine, Dr. Ri works with patients experiencing arange of chronic conditions, including digestive disorders. Whilehis clinic does not directly “treat” digestive diseases, the aim isto reduce nerve irritation and optimize nervous systemfunction—sometimes leading to surprising improvements in gut healthand overall wellbeing.
For those living with persistent digestive challenges, thejourney can be frustrating and isolating. Finding a clinician wholistens, considers the whole person, and collaborates with otherproviders can make all the difference. Many health insurance plansnow recognize certain forms of chiropractic care as part of abroader strategy for managing chronic conditions.
If you’re considering a new approach to digestive health, it’swise to consult your primary care provider and ensure all optionsare on the table. And remember: no single therapy fits everyone.The path to relief is often winding, and sometimes, it requires abit of experimentation and an open mind.
References & Further Reading
Ader, R., Cohen, N., Felten, D. "Psychoneuroimmunology:Interactions Between The Nervous System and The Immune System."Lancet 345:99-103, 1996.
Black, P. "Immune System–Central Nervous System Interactions."Antimicrobial Agents and Chemotherapy 38:7-12, 1994.
Eriksen, K. Upper Cervical Subluxation Complex – A Review of theChiropractic and Medical Literature. Lippincott, Williams &Wilkins, 2004.
Heitkemper M, Burr RL, Jarrett M. "Evidence for autonomic nervoussystem imbalances in women with irritable bowel syndrome." Dig Sci1998.
National Institutes of Health. "Irritable Bowel Syndrome." NIH IBSFact Sheet
Mayer EA, et al. "Gut/brain axis and the microbiota." J ClinInvest. 2015.
For appointments or more information, you can reach Dr. JeromeRi, DC at (714) 848-8122, or use the clinic’s online contactform.
Digestive disorders can be relentless, but new research andintegrative care models are helping more people reclaim theirhealth—sometimes in ways that defy simple explanation. The journeyis rarely linear, but with the right support, many find their wayback to a life less dominated by digestive distress.





Leave a comment